Why did I chose to start my cancer treatment in a hospital 200 kilometres from my city that has a perfectly good hospital that treats cancer?
My GP with the nervous, wry smile when announcing my diagnosis said… “You would be crazy to do that! Our hospital has great oncology and radiotherapy departments. I know the head of the team. He is a great guy. The surgeons are good. But you would be mad to go to Melbourne! Our city has better survival rates, and if you were my sister I would say you’d be mad to do that!”
There was criticism from others too.
Let me see, my breasts, my body, my mind, my life! There is a lot more to lose when you look at it from my perspective.
We had the roofs of our houses fixed last year and I stupidly accepted the first and only quote. So I have learnt the hard way. Why would I get one quote relating to something so important? This is a very serious matter and I didn’t want to look back in years time and ask the question would the outcome have been any different had I gone to a large specialist cancer hospital in a the big smoke? So I did some research.
In my future, the outcome of this decision may be no different. But I am happy with the decision I have made. I will have all of the surgeries in Melbourne, the treatment plan will be decided on by a large team of professionals and referred back to my local hospital where I will undergo chemotherapy and radiotherapy five minutes drive from home.
But the decision about treatment is a deeply personal and individual one.
In Australia, people have a choice to be covered by their own private health insurance scheme or the publicly funded government system called Medicare. Philosophically and practically, my husband and I have always been opposed to private health. Partly because we have never been able to afford it, living on single incomes as each of us studied or raised our family or paid our HECs debts, or met the expenses of our generation X living. We also, like many, got tangled in the large net of home ownership dreams that has been sold to many Australians. I guess it’s about priorities. But a user pays health system that gives greater healthcare access to people who can afford it just does not sit well with me.
I often wonder what would be my predicament if I lived in the United States and had the same living arrangements, but with the added burden of medical bills showing up in our letter box. Could I claim a redback spider living in the letterbox bit the hand of the postman and so prevented him for delivering such bills? Obviously not. Redbacks do not live in the United States! But seriously, to have to open a letter that says $1500 for the scan, $900 for this, and $450 for the specialist appointment that lasted 28 minutes would be devastating. Or in days gone by, I might have had to mortgage my house to have access to available medicines for breast cancer treatment (as was the case when Herceptin was first introduced in Australia). Heartbreaking stories. I just don’t know how my mental health would fare if this was my reality. It is true, treatment does not come cheap in either country. And if we had chosen private health insurance there would be the actual ongoing costs as well as the gap costs which also add up.
I cannot even begin to fathom what this whole experience might be like living in a developing nation where cancer rates are following similar patterns as here, albeit without the technology, supplies and the standard of medical care we take for granted.
So I am very, very, very fortunate.
Why should access to healthcare ever be about socio-economics? I have never been able to wrap my head around that. Feel free to call me an idealist. Friends have said… “But what happens to you or the kids in this public system if one of you needs a hip or knee replacement? You will have to wait for years in the public system and what if you have cancer?”
Cancer? Cancer is not a problem!
Yesterday, my results from the surgery where completed by the pathology team. They were printed and collated. I’m hoping the breast tissue and all of the nodes cooperated. The results were emailed to all relevant team members. Sometime in their busy day of rushing to patient clinics and ward rounds with takeaway coffee cups they would have taken a look.
Some of the members of my illustrious team work most of their week in the private hospitals nearby and they run through the parks to work at my public hospital. I’m not sure about it, but I think my breast surgeon runs in her stilettos across Fitzroy Gardens. One day I might go and sit there quietly under a tree on a park bench along the main path between the private and public hospital she goes between. I would need to be incognito, but it would help me confirm if she does in fact do this. That might be a bit obsessive and stalkerish? Hmmm, only if people find out about it, I guess.
So, this team, my team, met to review my case yesterday. In the room there were up to fifty health professionals who listened to the presentation and reviewed all the data. They might have debated and they hopefully reached a consensus on the best course of treatment for me. Patient is Lisa. She is 37, almost 38 years old, has two very young gorgeous children and an awesome husband, has a healthy BMI, is physically active, likes running and triathlons and chocolate, bloods results are good, comes to appointments well researched and asks lots of questions, doesn’t let much slip by her. Actually, probably none of this is mentioned, more like… staging scans clear so far, full pathology results are… cancer type, tumour size, grade, margins, hormone status, HER2 status, nodal involvement. The surgeons provide a brief, the plastics team representative says something, the nurse coordinator says something then the oncologists discuss my treatment plan. Discussion. Alternatives? Consensus reached? Great! Next patient…
So when I worried about getting a second opinion in the early days and stressed over my decision to go to the capital city because I really, really wanted a second opinion, I never dreamed I would essentially be given between five and fifty of them. One can never collect too many opinions!
I wanted to be there in this meeting. After all, it is me they are talking about. But the hospital has a policy of not allowing patients to be present. Apparently they trialled patient involvement in these review meetings recently and it didn’t fare so well. The outcome of the trial was that patients don’t like to see professionals debating treatment options. They don’t like to see time wasted on discussion about rounds of golf or a new restaurant that just opened in the CBD. Or flirting between colleagues. Patients don’t like to see uncertainty. They don’t want to know that oncological treatment options could go several ways based on research studies and differing opinions. They don’t want to see personalities and institutional politics or pecking orders at work. What if the bully oncologist wins the argument, not out of merit, but an ability to stomp on the views of others? What if they are tired in this meeting? It is someones life we are talking about isn’t it? My life.
This doesn’t worry me. Like all things, medicine is culturally constructed. It is the best tool we have in dealing with these matters. But I don’t prescribe to the notion that there is the best and most undisputed way. Our understanding of the world is changing all the time. And thank God it does. Cancer treatments evolve and change all the time. And it is through this dialogue between practitioners and their research debate that we know more and more. I am accepting of this whole process.
I would have really appreciated an invite but alas I didn’t receive one. So as would have it, my ears burned a little yesterday.
I imagined the room would have been full of crazy ties, business shirts, perfume and beards, spectacles, after shave and Audi key-rings. Clipboards, pens, iPhones, iPads and perhaps some egos. But most importantly the room would have been filled with (at the very least), a collective 500 years of medical knowledge and experience in both public and private healthcare and there can be no price put on that.
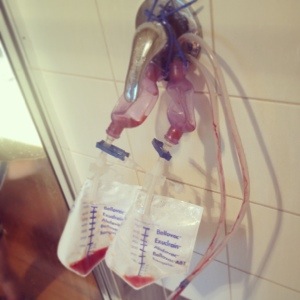
I have enjoyed the nurse at home visits. This week I met five awesome people who assisted me in the home with their bag of hospital latex gloves and Tegaderm dressings to see how I am faring and to measure my drain output. All of them work part time visiting patients in local homes and spend the bulk of their week in the emergency department, or paediatrics or other hospital departments. The home visits help them get out for a while and keep them fresh. One of the Exudrain twins has now been removed and the second will get to go on a car ride back to Melbourne tomorrow for the much anticipated results. Once it is out I will be free!
After a week of struggling with breakthrough pain at night time, I got on top of it yesterday. My awesome GP who isn’t so good at telling his patients about the cancer within them, is very good at writing a script to restock my supply of Endone. It would also appear he is great at checking my post diagnosis triathlon result online. So we are all cool again. It was never going to be an easy task for him, being the deliverer of such bad news.
Life is good.

Best of luck tomorrow Lisa I hope all good things come your way sleep well don’t stress
LikeLike
Thinking of you and praying for good results Lisa. X
LikeLike